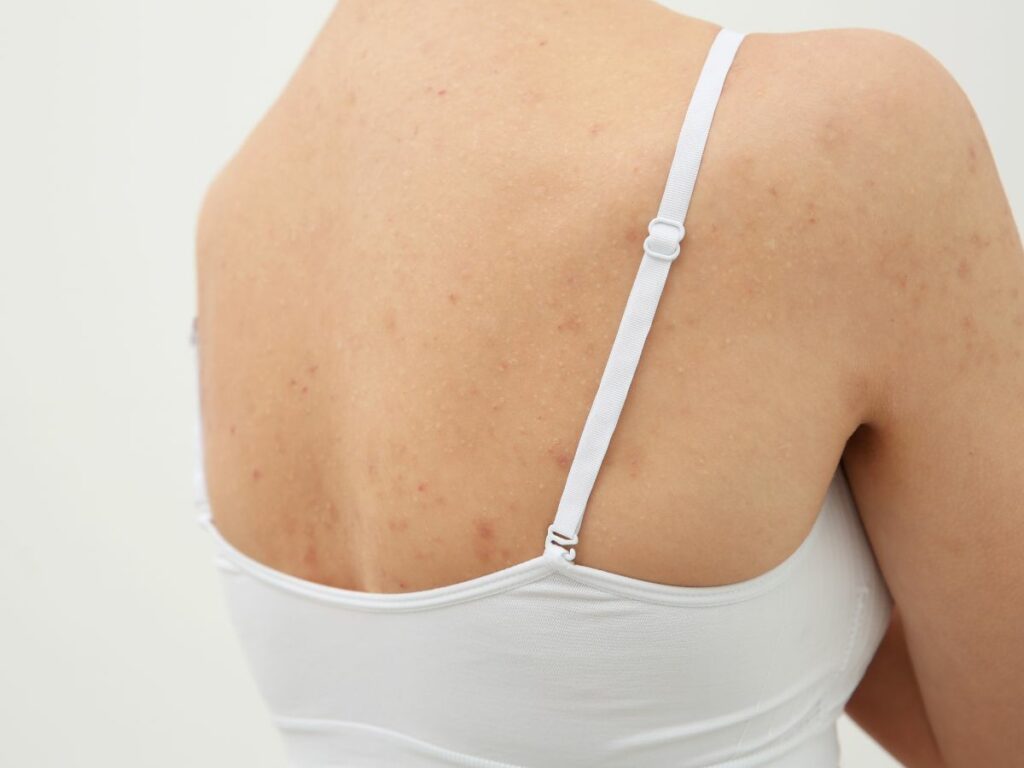
If you’ve been struggling with breakouts, and none of the advice you try seems to work, it could be that the pimple-like lumps on your skin aren’t acne at all – they could be fungal ‘acne’. Keep reading to learn more about this condition: what it is, how it differs from real acne, and what to do if you think you have it.
What Is Fungal Acne?
First of all, the condition popularly called fungal acne is not acne at all, but fungal folliculitis, an inflammation of the hair follicles caused by an overgrowth of fungus. The fungus in question is the Malassezia yeast (yeast is a type of fungus), and this kind of folliculitis is sometimes called Malassezia folliculitis or Pityrosporum folliculitis. But by convention, it’s often called fungal acne due to its superficial similarity to real acne, even by experts who know what it really is.
What Causes Fungal Acne?
Malassezia furfur is naturally present on the skin of about 90% of people. Usually, it causes no trouble and lives in harmony with the other fungi and bacteria that live on your skin, but it can grow out of control given the right environment and circumstances. Certain things can throw out this natural balance and cause Malassezia yeast populations to explode, leading to fungal acne.
Factors that can contribute to yeast overgrowth leading to fungal acne include:
Warm, Humid Climates
Since it’s a fungus, Malassezia yeast grows particularly well in places where the weather is warm, and the air is moist, just like mushrooms do.
Trapped Moisture
Similarly, anything that traps moisture close to your skin, like wearing sweaty clothes for too long after exercise (especially if they’re tight, or in fabrics that don’t breathe), will provide a hothouse environment that enables the growth of Malassezia.
Immune-Suppressing Medications
Certain medications, including corticosteroids, are used to treat health conditions in which the immune system attacks the body’s healthy tissues. These medications work by suppressing the immune system, which can have the side effect of allowing organisms like bacteria and fungi to grow out of control. This situation can lead to fungal acne and other infections.
Antibiotics
It’s common to get an outbreak of fungal acne after you finish a course of antibiotics. As well as killing the bad bacteria that cause bacterial infection, antibiotics kill the good bacteria (antibiotics only target bacteria; they don’t affect fungi). These good bacteria usually live in balance with the yeast that naturally lives on the skin, and without the bacteria there, yeast can multiply, causing fungal acne.
A Weakened Immune System
In addition to medications, your immune system can be weakened by health conditions, including diabetes and HIV, leaving your body more vulnerable to fungal, bacterial and viral infections.
A Fungus-Friendly Diet
Yeast feeds on sugars and carbohydrates, and eating too much of these fuels the yeast that causes fungal acne.
Oily Skin
Malassezia yeast feeds on oil, so oily skin creates a more hospitable environment for it to grow, whether it’s the sebum naturally produced by your skin or the oil in heavy skincare products.

Is Fungal Acne Contagious?
No, there are some forms of folliculitis that you can spread to other people, but fungal acne is not one of them.
Who Is Most Likely To Get Fungal Acne?
You have a greater likelihood of getting fungal acne if you:
- Live in a hot, humid climate
- Have a weakened immune system
- Take immune-suppressing medications
- Take antibiotics
- Are a teenager, because of the higher oil production of teenage skin
- People who use lots of skincare products that contain oil
- Are male: fungal acne is more common in males, although it does occur in females
What Are The Symptoms Of Fungal Acne?
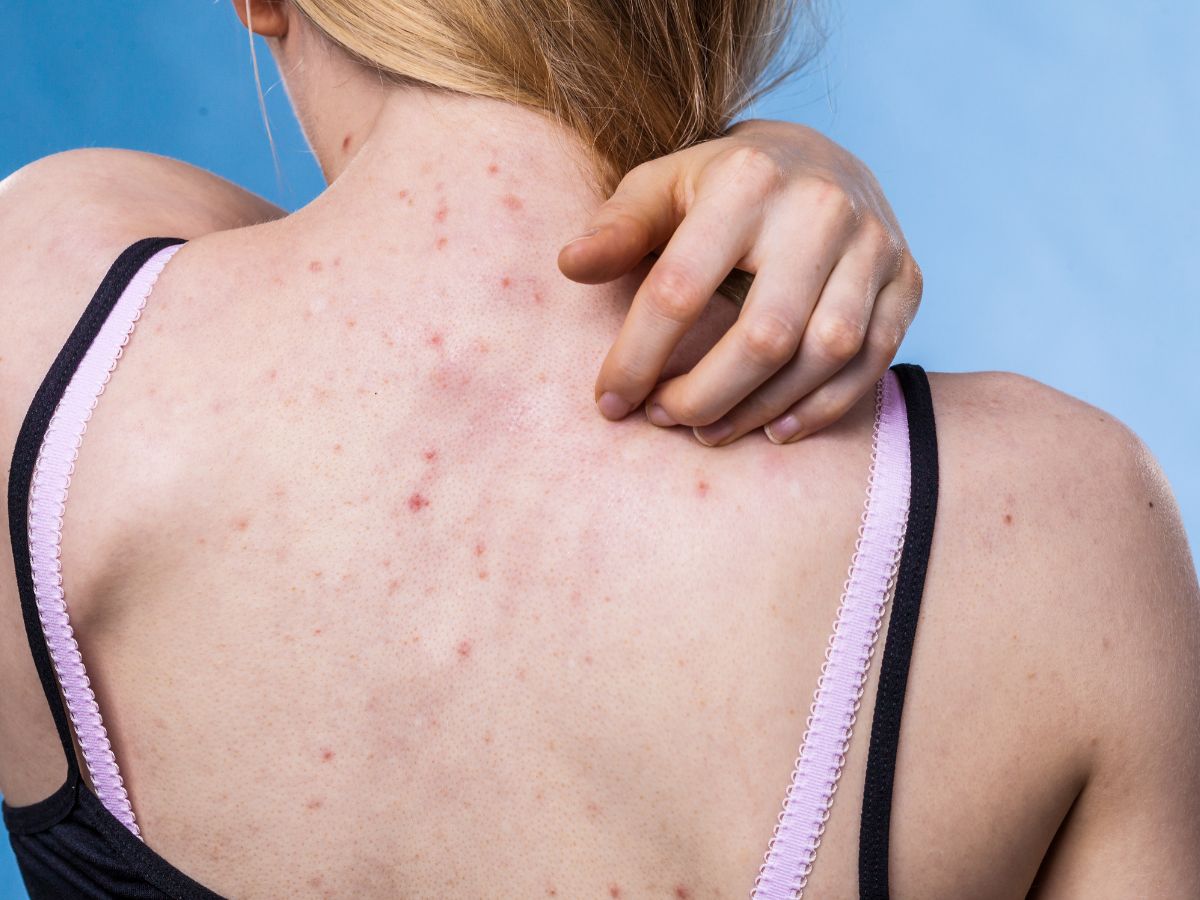
Fungal acne is marked by clusters of small, red bumps (papules) on your skin. Sometimes, they may have white heads filled with pus (pustules), making it easy to confuse them with regular acne (acne vulgaris). Whatever fungal acne bumps look like, they’re often very itchy.
What Is The Difference Between Fungal Acne And Normal Acne?
So if both fungal acne and normal acne cause red lumps, which may or may not have white heads, what’s the difference?
Under Your Skin
Human skin is covered with holes called pores. Each of these pores is the opening of a canal, called the follicle, through which a hair grows (there is usually just one hair per follicle, but not always). There is a gland secreting oil into the follicle from inside, the sebaceous gland (the oil it produces is called sebum). This oil travels up the follicle and out of the pore to reach the surface, forming a protective layer on the skin to keep it from drying out.
How Regular Acne Forms
Normally, sebum reaches the skin’s surface with no problem. But sometimes, the follicle can get blocked with a mix of dead skin cells and excess oil. This blockage allows a normally-occurring bacteria called Cutibacterium acnes (formerly called Propionibacterium acnes) to grow out of control and causes lumps called comedones. Comedones may be red due to inflammation in the follicle and may have a white, pus-filled head.
How Fungal Acne Forms
Like regular acne, the fungal folliculitis that we commonly call ‘fungal acne’ involves inflammation inside the hair follicles. Its appearance resembles regular acne, presenting as red lumps, sometimes with pus-filled heads. However, fungal acne is not caused by a blockage of oil and dead skin cells that allows bacteria to flourish. Instead, it’s caused by an overgrowth of Malassezia yeast, a type of fungus, inside the follicle. This, in turn, causes inflammation, and the inflammation causes the redness, itching and acne-like lumps that typify fungal acne.
In regular acne, inflammation in the follicle is a possible symptom caused by the blockage. In fungal acne, the inflammation in the follicle is the point – the ‘itis’ in folliculitis means inflammation. Remember, real acne is bacterial, not fungal – topical antibacterial treatments like the sprays and creams you might find in your first aid kit won’t necessarily have much of an effect against these organisms. There are bacterial forms of folliculitis, but they are caused by different bacteria than that which causes acne.
Indications You Might Have Fungal Acne Rather Than Normal Acne
Of course, only a doctor can diagnose you with fungal acne (or, rather, Malassezia folliculitis), but if your ‘acne’ shows a few of the characteristics below, it can indicate your skin problem is fungal rather than bacterial.
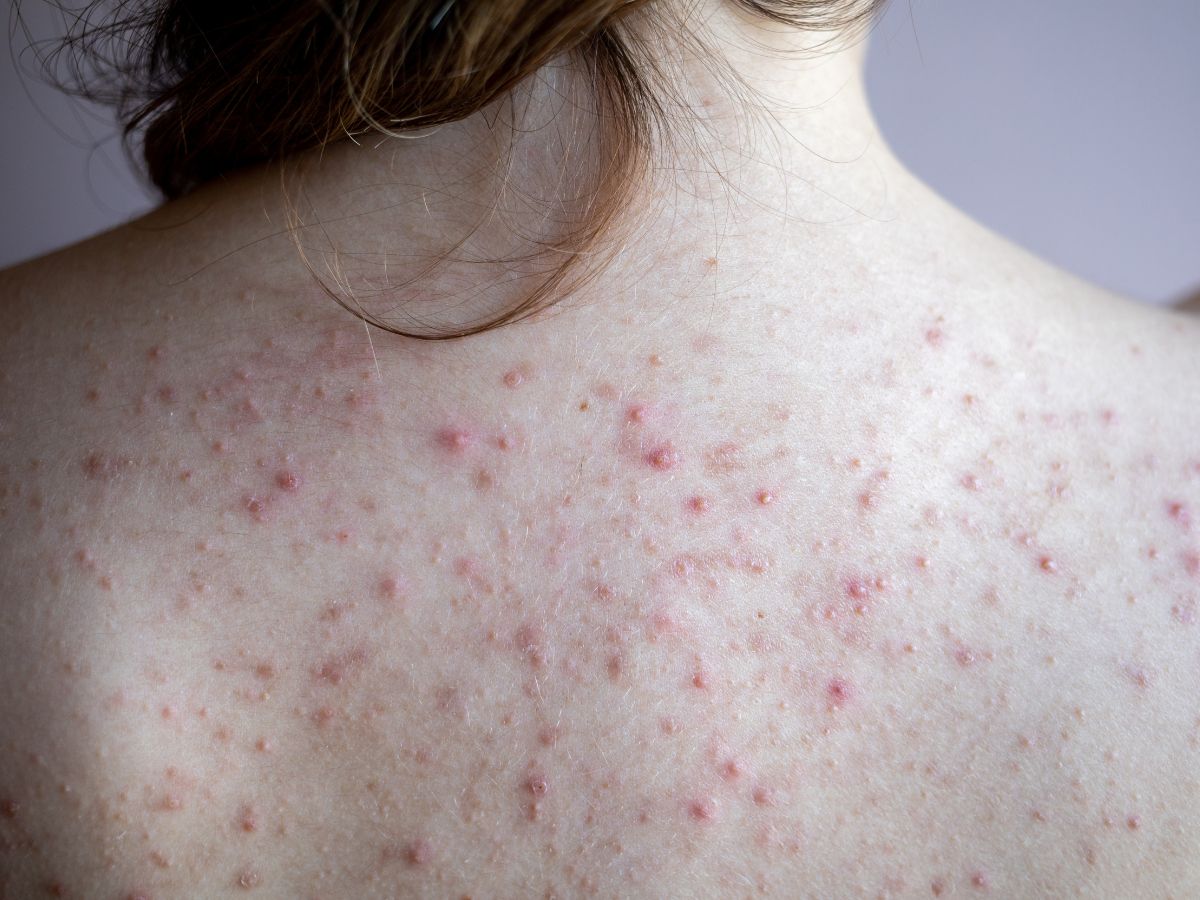
Size
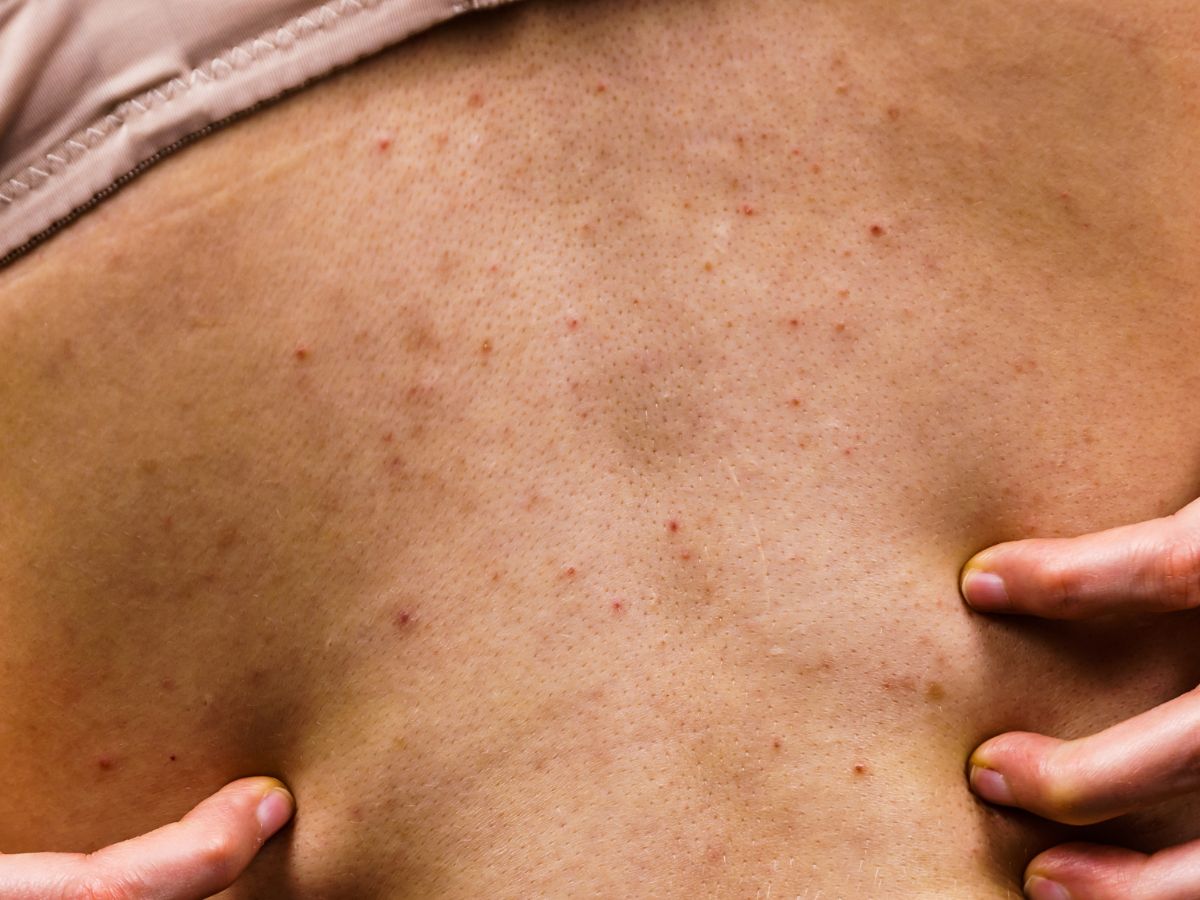
Fungal acne bumps are usually tiny, only one or two millimetres across. Real acne varies from tiny pimples to large pustules and nodules.
Uniformity
Fungal acne papules and pustules are usually very similar in size. With real acne, you may get pimples of different sizes in the same area at the same time.
Location
Fungal acne can occur anywhere where there are hair follicles but is most common on the upper chest, upper back and arms. Less commonly, it may occur on the face. Real acne is most common on the face but can appear on other body parts like the back and chest.
Itching
Fungal acne is typically very itchy. It’s uncommon for real acne to itch at all.
Clusters
Fungal acne usually takes the form of small lumps clustered together in groups. Real acne may cause multiple lumps in the same area, but these are usually more sparsely distributed.
Presence Of Other Fungal Problems
It’s fairly common to have other fungal skin conditions, like psoriasis, at the same time as fungal acne, as both are a result of yeast overgrowth. If you have a sudden growth of acne-like lumps and you’re experiencing other fungal skin conditions, it could indicate that the lumps are fungal acne.
Doesn’t Respond To Treatments For Regular Acne
Treatments that work well for real acne are usually targeted at removing dead skin cells that cause blockages, fighting bacteria, or both. They aren’t meant for dealing with the yeast that causes fungal acne.
Doesn’t Respond To Antibiotics
Doctors often prescribe antibiotics for persistent cases of real acne, and this treatment is often successful. If you are prescribed antibiotics for acne, but they don’t help or make the problem worse (or if your ‘acne’ cropped up for the first time after a course of antibiotics), you could have fungal acne.
How Is Fungal Acne Diagnosed?
When the time comes to get a formal diagnosis of fungal acne (or, more accurately, Malassezia folliculitis), the job can be done by a general practitioner or a dermatologist. They will arrive at a diagnosis by:
- Interviewing you about your symptoms. They may ask you about when the breakout began, what symptoms you’re having and what you’ve tried using to treat it.
- Examining your skin. As well as looking at your skin with the naked eye, they may use a special device called Wood’s light that can detect a fungal infection and several other conditions.
- Taking samples. To confirm the presence of Malassezia yeast, a doctor may take a scraping of your skin and look at it under a microscope or take a biopsy and send it to a lab.
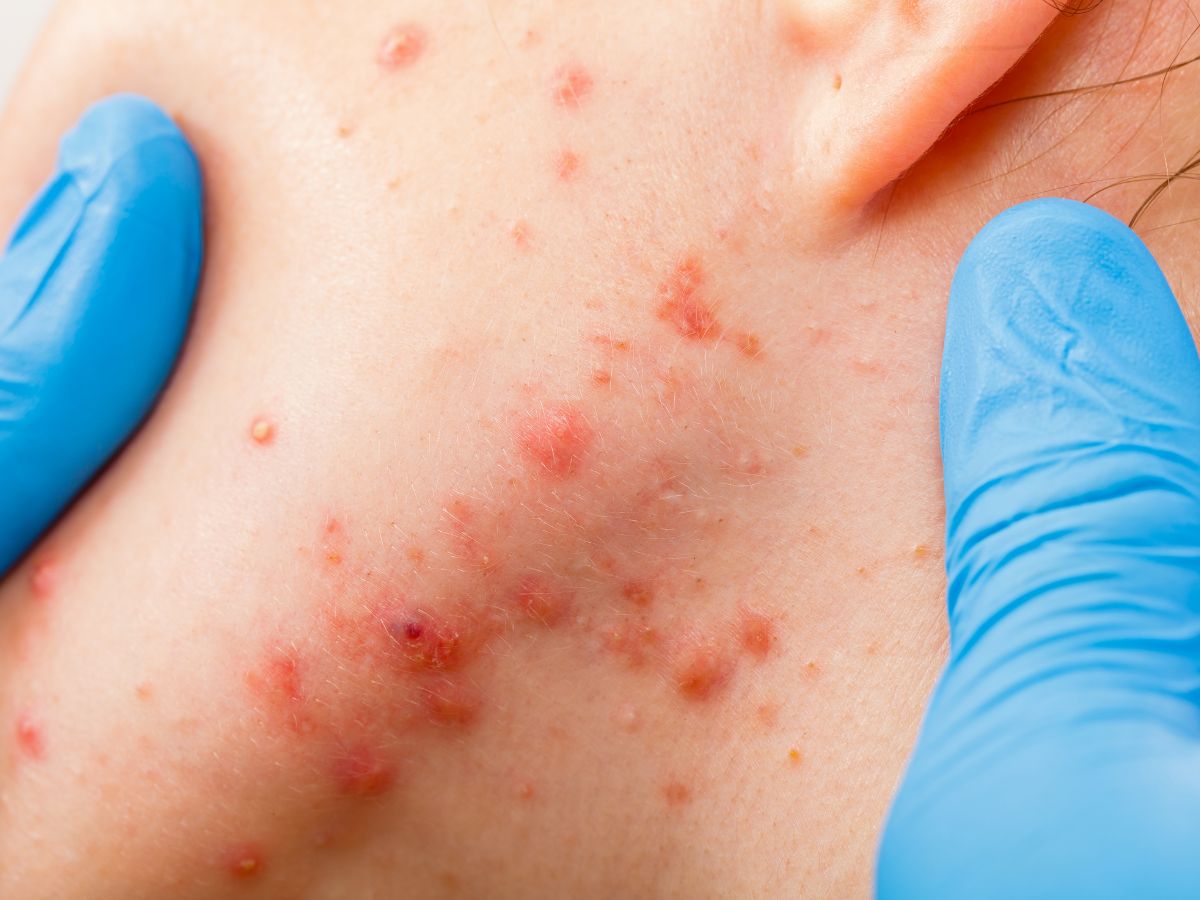
Other Types Of Folliculitis
Malassezia folliculitis (fungal acne) is only one type of folliculitis. Bacteria, mites, viruses or physical irritation can also cause inflammation of the hair follicles.
Superficial Bacterial Folliculitis
This is the most common form of folliculitis, usually caused by the bacteria Staphylococcus aureus. Like Malassezia, this bacteria is normally present on many peoples’ skin, but if follicles get damaged, it can get in there and develop into an infection. This kind of folliculitis can be spread to others by direct body contact or sharing razors.
Folliculitis Decalvans
Folliculitis decalvans is a rare type of folliculitis usually found on the scalp, which can lead to scarring and permanent hair loss. There is no clear consensus about the cause, but it may result from a reaction to Staphylococcus aureus.
Viral Folliculitis
As well as being fungal or bacterial, folliculitis can be viral, like hand, foot and mouth disease. Viral folliculitis is caused by the same virus responsible for cold sores, the herpes simplex virus. This condition is called herpetic folliculitis, and it can be spread by shaving.
Gram-Negative Bacterial Folliculitis
Sometimes called ‘hot tub folliculitis’, this form of folliculitis can appear after using poorly-maintained pools or spas. It’s caused by a specific type of bacteria, and other risk factors include having a weak immune system and long-term antibiotic use.
Demodex Folliculitis
Also known as demodicosis, this form of folliculitis is caused by a mite that lives on most people’s skin without causing any trouble, the Demodex folliculorum. On some people, this mite can lead to an irritating form of folliculitis.
Eosinophilic Folliculitis
Eosinophilic folliculitis is often found in people with HIV and can sometimes be a side effect of chemotherapy. Its exact cause is unknown.
Pseudofolliculitis Barbae
This type of folliculitis is caused by mechanical irritation rather than an infection. Pseudofolliculitis barbae mostly affects men with curly hair who shave – the hair shaft curls back into the skin, causing an irritating reaction that can present as red, brown or skin-coloured lumps in the area affected.
How Do You Treat Fungal Acne?
The first step in treating suspected fungal acne is addressing the problem at home with lifestyle changes.
Shower More Often
Taking more frequent showers can make a difference if you exercise regularly or have a job where you sweat a lot. Try taking a shower immediately after work or after you exercise, and then changing into clean clothes. This can help to control any yeast that may have begun to multiply in the warm, sweaty environment provided by your clothes.
Wear Looser Clothes
Tight clothes can restrict airflow around your body, creating a hospitable environment for yeast to grow, not to mention the friction against your skin that can further irritate your follicles. See if wearing looser clothing in breathable fabrics like cotton improves your fungal acne.
The next step in treating what you think might be fungal acne is to try over-the-counter treatments.
Over-The-Counter Antifungal Creams
Look for creams containing antifungal ingredients like econazole, ketoconazole, butenafine and clotrimazole, like those marketed for tinea and other fungal infections. Ask your pharmacist for advice.
Dandruff Shampoos
A common off-brand use for anti-dandruff shampoos is as a cleanser to treat fungal acne – they often contain fungus-fighting ingredients like ketoconazole and selenium sulfide. To get the most out of this treatment, you’ll have to leave the shampoo on the affected area for a few minutes before washing it off. It may be a good idea to try it on a small area first.
When Should I See A Doctor About Fungal Acne?
If, after three weeks, you’ve had no success treating what you think is fungal acne at home, it’s time to see a doctor. You should also see a doctor immediately for any rash you have that’s accompanied by a fever and general feelings of being unwell. Learn more about dealing with sudden health issues by enrolling in a first aid course.
If your doctor does diagnose you with fungal folliculitis, they may try the following approaches.
Oral Antifungal Medication
Sometimes the fungus is too deep in the follicles for topical treatments to be effective. To target the problem, a doctor may prescribe an antifungal medication to be taken orally, like fluconazole or itraconazole.
Photodynamic Therapy
Photodynamic therapy (PDT) is a treatment used for a wide variety of conditions, from fungal skin problems like psoriasis to various forms of cancer. In this technique, a doctor first administers substances that sensitise the skin to light either topically, orally or intravenously. Then a special light is applied to the treatment area. Photodynamic therapy is showing promise as a treatment for Malassezia furfur, the yeast behind fungal acne.
How Can I Manage The Symptoms Of Fungal Acne?
Aside from trying some of the over-the-counter topical solutions above, you can put a warm compress on the area to calm the inflammation and reduce your urge to scratch.
Will Fungal Acne Come Back After It’s Treated?
Although topical and oral treatments for fungal acne are effective, the condition can come back even after being successfully treated. You can reduce the risk of a recurrence by trying the advice for preventing fungal acne below. You could also consider regular use of topical treatments, like antifungal shampoo. Your doctor might have recommendations of their own about this kind of preventative treatment, or in the case of repeated breakouts of fungal acne, might even prescribe long-term use of antifungal medications.
How Do You Prevent Fungal Acne From Recurring?
There’s no guarantee that fungal acne will stay gone after treatment, but you can reduce the risk of another outbreak by taking the steps below.
- Wash your face twice a day.
- Don’t use moisturisers or sunscreens that are too oily.
- Consider using a dandruff shampoo with antifungal ingredients as a body wash regularly.
- Try to avoid shaving every day, as this can further irritate the already-inflamed follicles.
- Wear looser-fitting clothing, preferably in breathable fabrics, especially in hot and humid weather or during exercise.
- Shower and change your clothes immediately after you work out.
- While you’re at it, wash your sweaty fitness gear immediately after wearing it.
- If you swim, wash your bathing suit and let it dry after each use.
- Eat a balanced diet without too many carbohydrates and sugary foods, as yeast feeds on these.
Conclusion
You should now have more of an idea about whether those persistent pimples are acne or fungal folliculitis, and if it looks like you do, you also have a few suggestions to try at home. If the problem is too difficult to manage on your own, or if you have a skin condition and you feel sick or have a fever, see a doctor. To learn more about responding to health problems, enrol in an accredited first aid course.