Hand, foot and mouth disease is a very common childhood illness. In fact, only a few people will reach adulthood without experiencing its unpleasant but mostly harmless effects. Whether you’re the parent of a patient or one of the rare adults to suffer through the blisters and mouth sores that are part of the illness, find out all you need to know about the causes, symptoms and treatment of this widespread disease below.
What Is Hand, Foot And Mouth Disease?
Hand, foot and mouth disease (enteroviral vesicular stomatitis, HFMD or HFM) is a viral illness common in children under the age of 10. Its name comes from the characteristic rash it causes, which often appears on the hands, feet and mouth but can be found elsewhere on the body. Outbreaks of HFMD frequently occur in warmer weather and are more common in certain parts of the world, like Asia.
Hand, Foot And Mouth Disease vs Foot-And-Mouth Disease – What’s The Difference?
Foot-and-mouth disease affects livestock and is rarely passed to humans, and hand, foot and mouth disease affects humans and can’t be passed to animals.
What Causes Hand, Foot And Mouth Disease?
Hand, foot and mouth disease is caused by viruses from the enterovirus family, usually, a strain of the coxsackie virus, coxsackievirus A16 (CA16) being the most common. Other enteroviruses that can cause include enterovirus 71 (EV-A71 or EV71), which is more likely than CA16 to cause serious complications.
How Does Hand, Foot And Mouth Disease Spread?
Hand, foot and mouth spreads through contact with an infected person’s bodily fluids and wastes. These substances could include saliva and mucus (especially airborne droplets generated by coughing or sneezing), faeces, blood, or fluid from popped blisters. HFMD blisters cease to be infectious when they dry up. Contact with fluids carrying HFMD can be via the infected person or a surface they have had contact with.
Who Is At Risk Of Hand, Foot And Mouth Disease?
Children under the age of 10 are most vulnerable to hand, foot and mouth disease, and it spreads rapidly in environments like schools and childcare centres where children play games together and share toys.

Can Adults Get Hand, Foot And Mouth Disease From A Child?
Children usually gain some immunity to hand, foot and mouth after exposure to the virus, which is why it becomes less common after the age of ten (most people have been infected by the time they’re old enough to start worrying about atherosclerosis). However, it is possible for an adult to get hand, foot and mouth disease, especially if their immune system is weakened.
What Are The Symptoms Of Hand, Foot And Mouth Disease?
Symptoms of hand, foot and mouth disease may resemble those of the flu, including:
- Fever
- Runny nose
- Sore throat
- Tiredness
- Irritability
- Enlarged lymph nodes in the neck
The rashes and blisters that come with HFMD may appear a few days after the flu-like symptoms, and depending on which specific virus caused the infection, may take the form of:
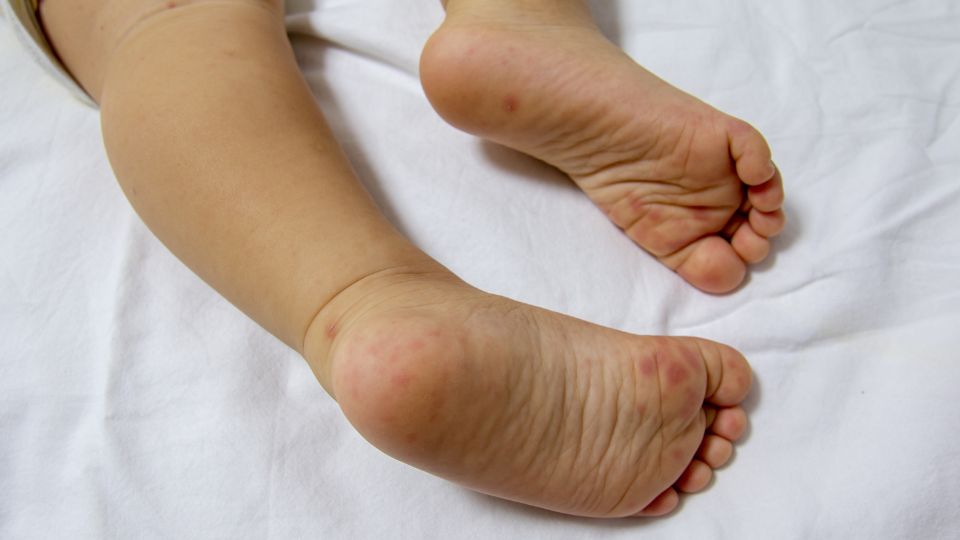
- Small, white blisters on the palms of the hands, the soles of the feet, inside and around the mouth
- A red rash with a brown, scaly texture on the surface of the limbs, hands, feet, around the mouth and the buttocks.
How Is Hand, Foot And Mouth Disease Diagnosed?
A doctor will usually diagnose hand, foot and mouth disease by looking at the rashes and blisters and interviewing your child about other symptoms. Occasionally, they may also take samples for testing, including throat swabs or stool samples.
What Are The Potential Complications Of Hand, Foot And Mouth Disease?
People with hand, foot and mouth disease almost always recover within 10 days with little or no treatment, but there can be complications on rare occasions.
Dehydration
Children may find it hard to get enough liquids if painful sores are inside the mouth, which can result in dehydration. Parents should take care that they drink enough and look out for the warning signs:
- Dry lips and tongue
- Dry skin
- Cold hands and feet with a blotchy appearance
- Drowsiness
- Rapid breathing
- Sunken eyes
- A sunken soft spot (fontanelle) on top of the head in babies
- Dark yellow urine
- Fewer wet nappies
- Fewer tears when crying
Children with sores inside their mouths may find cold drinks soothing, and some commercially-available drinks meant for treating dehydration are also available as ice blocks.
Loss Of Fingernails Or Toenails
Sometimes fingernails or toenails may fall out shortly after a bout of hand, foot and mouth disease, but doctors can’t confirm that the illness is the reason for this. In any case, when nails are lost after HFMD, they typically grow back on their own.
Serious But Rare Complications Of Hand, Foot And Mouth Disease
Very rarely, hand, foot and mouth disease can cause serious complications, including encephalitis, meningitis, paralysis and myocarditis. These are not usually caused by coxsackievirus A16, the most common cause of HFMD. They are more likely to be caused by less common HFMD-inducing viruses, like enterovirus 71 or enterovirus D68.
| Complication | What It Is | Symptoms |
| Encephalitis | Inflammation of the brain | Fever, confusion, fatigue, headache, stiff neck, stiff back, nausea, vomiting, confusion, memory loss, aches in the muscles or joints, sensitivity to light, muscle weakness, problems with speech or hearing, personality changes, confusion, seizures, paralysis, coma In babies or younger children: A bulging fontanelle, not feeding well, stiffness over the whole body, irritability or fussiness |
| Meningitis | Inflammation of the membranes that cover the brain and spinal cord (the meninges) | Fever, sensitivity to light, stiff neck, severe headache, nausea, vomiting, fatigue, drowsiness, confusion, irritability, pain in the muscles or joints, bruising or blotchy red or purple rash that may look like small dots (especially if it doesn’t blanch when you press it with a glass), seizures, cold hands and feet In babies or younger children: Fever, a bulging fontanelle, unusual sleepiness, floppiness, feeding problems, an unusual cry, constant crying, vomiting, difficulty feeding, difficulty waking, yellow skin, a blotchy red or purple rash that may look like small dots (especially if it is non-blanching), pale or blotchy skin, arching their back, seizures |
| Acute Flaccid Myelitis | A neurological disorder caused by inflammation of the spinal cord | Sudden weakness of the arms and legs, paralysis (acute flaccid paralysis), slow or no reflexes, facial weakness, facial drooping, trouble swallowing, trouble breathing, slurred speech, headache, neck pain, back pain, changes in urination or bowel movements |
| Myocarditis | Inflammation of the heart muscle | Chest pain, breathing difficulties including rapid breathing, rapid or irregular heartbeat, fever, fainting, anxiety, failure to gain weight, producing less urine than usual, pale and cool hands and feet, abdominal pain and nausea, swelling in the legs, feet or face |
What Are The Early Signs That Hand Foot And Mouth Disease Is Becoming More Serious?
If your child shows any of the following symptoms, it could mean that their hand, foot and mouth disease is progressing to a more serious infection, and they are more likely to develop complications.
Seek immediate medical attention, even if you have had a previous medical appointment, if your child:
- Has severe symptoms
- Has not had an improvement in their symptoms after 10 days
- Has a fever lasting more than 72 hours
- Is breathing rapidly
- Is very tired
- Is very irritable
- Is having trouble walking
- Is immunocompromised
- Is becoming dehydrated – symptoms may include having sunken eyes or producing less urine than normal
- Is very young
- Has a severe headache
- Has stiffness in their neck or back
- Has a rash that doesn’t blanch (lose its colour) when you press on it
- Shows any other symptoms that concern you
Although it’s very rare for hand, foot and mouth disease to become serious in any way, you can be prepared for this or any other unexpected medical emergency by enrolling in an accredited first aid course.

What Is The Treatment For Hand, Foot And Mouth Disease?
Usually, no treatment is needed for hand, foot and mouth disease, and the patient recovers on their own within about ten days. But you can make the process less stressful for them by providing care and pain relief with items that may be in your home first aid kit or medicine cabinet:
- Over-the-counter pain relief, including ibuprofen or paracetamol (but not aspirin)
- Calamine lotion or a similar topical anti-itching treatment for rashes
- Non-acidic cold drinks or ice blocks to relieve a sore throat and any sores inside the mouth
- Likewise, gargling with warm salt water may help soothe soreness in the mouth and throat (if your child is old enough to spit it out afterwards)
- Get your child to sip on a drink frequently to stave off dehydration
- Do not pick or pop any blisters – the fluid inside them carries the virus. If they do pop, wash them with lukewarm water and soap and gently pat them dry before covering them with a sterile dressing
- Give your child soft foods that aren’t too hot or acidic (avoid things like tomato sauce
- Try to make sure your child gets plenty of rest
Will Antibiotics Help With Hand, Foot And Mouth Disease?
No. Antibiotics only work on bacterial infections, and hand, foot and mouth disease is viral, so antibiotics won’t work on it. What treatment will work on an infection depends on whether it is viral, bacterial or fungal.
Are There Any Drugs For Hand, Foot And Mouth Disease?
No, there are no drugs developed specifically for hand, foot and mouth disease. Treatment is focused on relieving symptoms while the body fights the infection.
Is There A Hand, Foot And Mouth Disease Vaccine?
Basically, no. There have been reports from China of a vaccine that is effective against one of the viruses that can cause hand, foot and mouth disease, enterovirus 71, but this vaccine is not available in Australia, and there are other strains of enterovirus that cause the disease, anyway. The best way of preventing HFMD is to practise good hygiene.
How Can Hand, Foot And Mouth Disease Be Prevented?
The following steps can reduce the risk of catching hand, foot and mouth disease:
- Wash your hands with soap and water after coming in contact with the bodily fluids of someone with hand, foot and mouth
- Clean and disinfect any clothing, surfaces or toys that have been in contact with the infected person
- Don’t share utensils, cups and plates
- Teach children proper hygiene for coughing and sneezing and how to wash their hands properly if they are old enough
- Avoid touching your eyes, nose and mouth
- Avoid close contact with sick people
How Long Is Hand, Foot And Mouth Disease Contagious?
Hand, foot and mouth disease is most easily spread within the first seven days of the illness, but there is a smaller possibility that it may be spread for a few weeks after the end of symptoms. The virus may be present in bowel movements for weeks after recovery, so extra caution will be necessary for small children who need to be changed, especially if they will be in an environment with many other children, like a childcare centre.
Should Children Stay Home From School If They Have Hand, Foot And Mouth Disease?
If your child has hand, foot and mouth, keep them home from school, daycare or any other place where they will be in contact with other children if they:
- Have a rash
- Have blisters filled with fluid (blisters that have dried up are no longer infectious)
- Have a fever
- Are drooling because of sores in their mouth
Once these symptoms have disappeared and your child feels well, it should be okay for them to return to school or daycare, but find out whether your school or daycare provider has any rules about this first.
Should I Go To Work If My Child Has Hand, Foot And Mouth?
If your child has hand, foot and mouth disease, you should stay home from work for as long as they have rashes and blisters, fever, sore throat or other symptoms.
Can I Go To Work If I Have Hand, Foot And Mouth Disease?
If you have hand, foot and mouth yourself, the same guidelines apply to you that apply to children staying away from school because of the illness: don’t go back until your symptoms (and your child’s) disappear and you feel well.
Does Hand, Foot And Mouth Disease Cause Any Issues During Pregnancy?
Pregnancy complications from hand, foot and mouth disease are very rare, but if you are pregnant and come in contact with someone with hand, foot and mouth disease or you get a rash of any kind, see your doctor. There is also a chance of passing HFMD on to the baby if you catch it late in your pregnancy, but most babies born with the illness don’t have severe symptoms.
Getting Ready For Your Appointment
Here are some things to remember as you prepare for your child’s appointment with the doctor, whether you’re doing so to get a diagnosis of hand, foot and mouth disease or you’re concerned about any changes in their condition.

What To Have Ready For The Doctor
- A list of symptoms, including those your child is no longer experiencing
- Your child’s medical history
- A list of any medications and supplements your child takes
- A list of questions you want to ask the doctor
- A pen and paper to write down any instructions
Questions You May Want To Ask
- What is causing your child’s symptoms
- Whether your child needs any tests
- How to manage any other conditions your child has along with this
- How to make your child more comfortable or relieve discomfort
- Whether there is anything you have to avoid
- Whether the doctor can recommend any resources like brochures or websites
Summary
You should now be well-prepared to deal with a case of hand, foot and mouth disease in the family, including dealing with painful mouth sores, preventing the spread of the disease to others and even recognising early on when something is not right, and further medical help is needed. If you want to be even better prepared for any medical issues your family might face, take the time to enrol in any accredited first aid course.


